Simple, Viable Republican Alternatives To Obamacare
Stanley Feld M.D., FACP, MACE
There are many simple and viable alternatives to Obamacare which Republicans should start considering.
Republicans should seriously consider My Ideal Medical Savings Account as an alterative to Obamacare. It is logical, simple, does not require a large complicated infrastructure and aligns all the stakeholders’ incentives.
It is easy for consumers to understand.
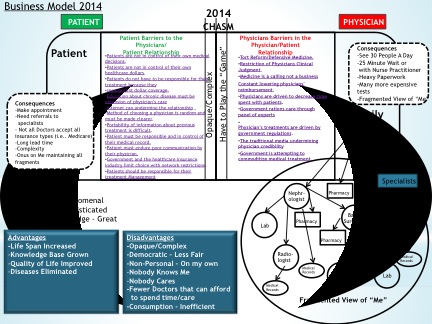
Consumers want to have choices. The dysfunction of our healthcare system has gotten to the point where most consumers don’t have a choice. Consumers simply do not know they lost their freedom of choice and access to care until they get sick.
Consumers think they have adequate healthcare coverage until they get sick. Only 20% of the population gets sick.
The other 80% of the population refuses to think about the problem.
When they do experience illness, the dysfunction in the healthcare system makes them furious. They want to blame someone. Physicians are usually the targets of their frustration.
Most physicians are trapped in a situation that causes them to fight for their own survival for all the reasons I have previously enumerated. This creates a more dysfunctional healthcare system.
All the stakeholders fight for their own vested interests. These vested interests have become misaligned. The vested interest of the government is to control of the system and decrease its costs.
Costs cannot be controlled by regulations without consumer involvement. Consumers of healthcare must understand the effectiveness of their care is dependent on their involvement in their own medical care.
Consumers’ adherence to treatment is a key component in the effectiveness of medical care.
Medical costs cannot be controlled by government price fixing.
Medical costs cannot be controlled by government restrictions to access of care. Consumers will become sicker resulting in a higher cost illness.
A functional healthcare system must provide financial incentives to consumers in order for them to want to be empowered to control costs. Consumers should not be dependent on the government to control costs.
The government must repair the actuary and accounting rules of the healthcare insurance industry. Insurance reserves should not be scored as a loss to justify premium increases.
The healthcare insurance industry takes 40 cents off the top of every insurance dollar that is spent. Consumers with both private insurance and government insurance are only getting 60 cents value for every healthcare dollar spent. The healthcare industry is allowed to do some strange accounting with their required reserves.
If this accounting method were repaired, premium costs would decrease.
Effective malpractice reform would result in a significant decrease in healthcare costs. The Obama administration refuses to believe tort reform is needed.
Many of the rules written into Obamacare, Medicare, and Medicaid are so screwy they defy common sense and penalize consumers. One glaring rule is Medicare permitting hospitals to admit Medicare patients to the hospital for observation for 48 hours.
Medicare does not pay for Observation admissions. Patients have to pay out of pocket for these admissions.
Consumers must become aware of these screwy rules and protest them. These rules have been written by the Obama administration to save the government money. These rules penalize patients the government professes to help.
Consumers are the only stakeholders that can motivate President Obama and congress to fix the significant points of waste in the healthcare system. Consumers have the power to vote.
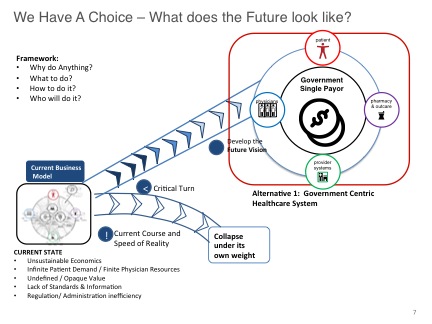
I do not believe that President Obama has an interest in repairing the healthcare system. All of his actions signify that he wants the healthcare system to fail. After it fails people will beg the government to completely take over and have a single party payer.
Does anyone trust the government to take over our most valuable asset, our healthcare?
The government take over will also fail because dependent consumers will figure out how to game the system just as food stamp recipient have figured out how to game that inefficient system.
The goal of a sincere administration and congress is to figure out how to motivate consumers to be “PROSUMERS” (productive consumer) with an economic interest in the healthcare system.
Airlines, banks, bookstores, entertainment venues have all figured it out. Why can’t the government help consumers figure it out?
It gives all Prosumers the incentive to be responsible for their health and healthcare dollars.
Below is the blog My Ideal Medical Savings Account Is Democratic!
My Ideal Medical Savings Account Is Democratic!
Stanley Feld M.D.,FACP,MACE
A reader sent this comment; “My Ideal Medical Savings Account (MSA) “was not democratic and leads to restriction of medical care for the less fortunate.'
This comment is totally incorrect. I suspect the comment came from a person who has “an entitlements are good mentality.”
I believe that incentives are good. They lead to innovation. Innovation leads to better ideas.
Healthcare entitlement leads to ever increasing costs, stagnation, restrict freedom of choice and decrease in access to care.
The excellent example of increasing costs, decreasing choice, and decreasing access to care is Medicaid.
The fact that someone is covered by healthcare coverage does not mean they have access to medical care.
I have written extensively about the virtues of My Ideal Medical Savings Accounts (MSAs). They are different than Health Savings Accounts (HSAs).
MSAs provide added incentives over HSAs to obtain and maintain good health. Obesity is a major factor in the onset of chronic diseases. Consumers must be motivated to avoid obesity to maintain good health. MSAs can provide that incentive.
The MSA’s can replace every form of health insurance at a reduced cost. It limits the risk to the healthcare insurance industry while providing consumers with choice.
This would result in competition among healthcare providers. Competition would bring down the cost of healthcare.
Some people might not like MSA’s because they are liberating. They provide consumers of healthcare with freedom of choice. They also give consumers the opportunity to be responsible for their healthcare dollars while providing them with incentives to take care of their health.
MSAs could be used for private insurance purchasers, group insurance plans, employer self- insurance plans, State Funded self-insurance plans and Medicare and Medicaid.
In each case the funding source is different. The cost of the high deductible insurance is low because the risk is low.
If it were a $6,000 deductible MSA, the first $6,000 would be placed in a trust for the consumer. Whatever they did not spend would go into a retirement trust. If they spent over $6,000 they would receive first dollar healthcare insurance coverage. Their trust would obviously receive no money that year.
The incentive would be for consumers to take care of their health so they do not get sick and end up in an expensive emergency room.
If a person had a chronic illness such as asthma, Diabetes Mellitus, or heart disease with a tendency to congestive heart failure and ended up in the emergency room they would use up their $6,000.
If they took care of themselves by spending $3,000 of their $6,000 trust their funding source could afford to give their trust a $1500 reward. The benefit to the funding source is it saved money by the consumer not being admitted to the hospital. The patient stayed healthy and was more productive.
President Obama does not want to try this out. He wants consumers and businesses to be dependent of the central government for everything.
MSAs would lead to consumer independence from central government control of our healthcare. MSAs would put all consumers at whatever socioeconomic level in charge of their own destiny.
The opinions expressed in the blog “Repairing The Healthcare System” is, mine and mine alone
Please have a friend subscribe
Republicans who really want to repair the healthcare system should take notice of these suggestions. They should stop proposing complicated alternatives to Obamacare that will not work.
Republicans should start trying to understand the real problems in the healthcare system.
The opinions expressed in the blog “Repairing The Healthcare System” is, mine and mine alone
Please have a friend subscribe